Oral Thrush Treatment Selector
This tool helps you determine the most appropriate treatment for oral thrush based on your specific situation. Select your conditions below to get personalized recommendations.
Select your conditions above to see your treatment recommendation.
Oral thrush isn’t just a nuisance-it can make eating, swallowing, and even talking painful. If you’re on long-term medications like inhalers for asthma, antibiotics, or immunosuppressants, you’re at higher risk. This isn’t rare. Around 5% of people get it at some point, but for those using inhaled steroids, the rate jumps to 20%. The culprit? A fungus called Candida albicans that normally lives harmlessly in your mouth-until your meds throw off the balance.
Why Medications Cause Oral Thrush
Some medications don’t just treat your condition-they disrupt your mouth’s natural defenses. Inhaled corticosteroids, like those in Advair or Flovent, are the most common trigger. They reduce inflammation in your lungs, but they also kill off the good bacteria that keep Candida in check. If you don’t rinse your mouth after using your inhaler, the residue sits there like a welcome mat for fungus. Antibiotics are another big one. When you take them for a sinus infection or strep throat, they wipe out both bad and good bacteria. Without enough good bacteria to compete, Candida takes over. Immunosuppressants used after organ transplants or for autoimmune diseases like lupus also lower your body’s ability to fight off fungal overgrowth. Even some cancer treatments weaken your immune system enough to let thrush bloom.What Oral Thrush Looks and Feels Like
It doesn’t always start with pain. At first, you might notice white patches on your tongue or inner cheeks that look like cottage cheese. They don’t rub off easily. If you scrape them gently, you might see red, raw skin underneath. As it gets worse, your mouth feels sore, dry, or burning. Swallowing becomes hard. Some people say food tastes metallic or off. In severe cases, the infection spreads down the esophagus, making swallowing painful or even impossible. You might think it’s just a sore throat or a cold, but if you’ve been on one of those medications and these symptoms last more than a few days, it’s likely thrush. Don’t wait for it to get worse.Nystatin: The First-Line Treatment
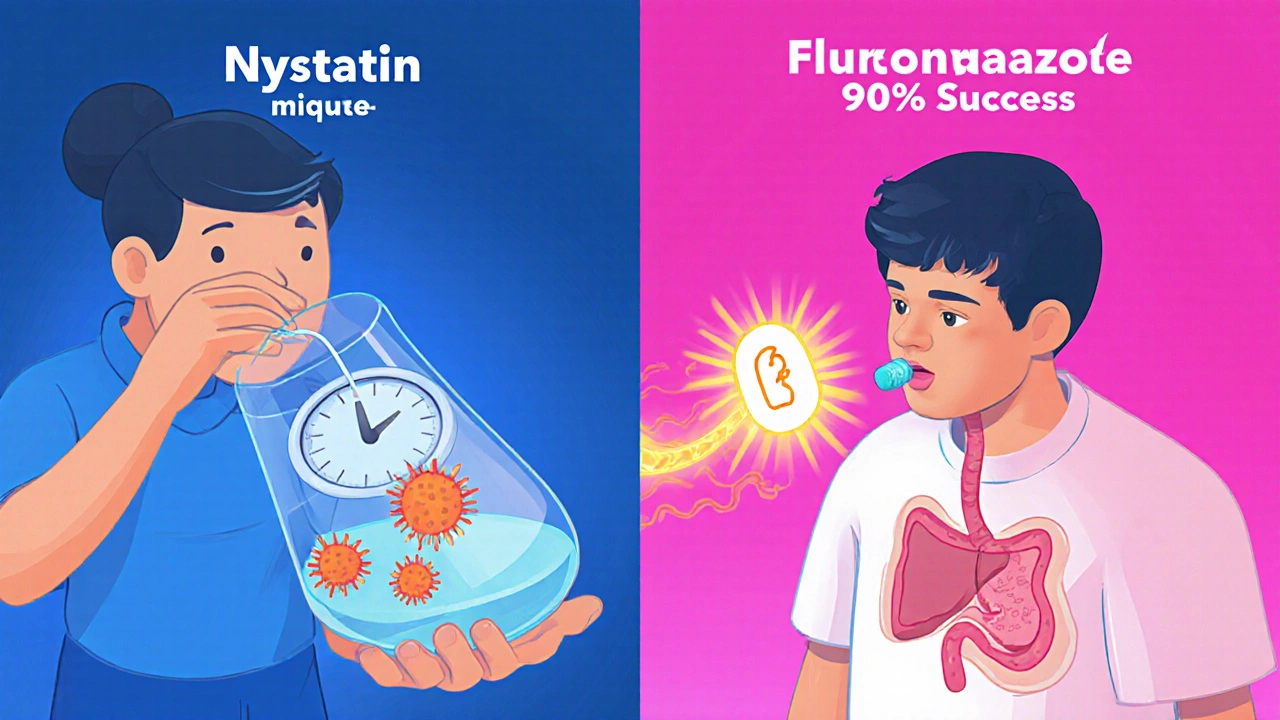
For most people, especially those who are otherwise healthy, nystatin is the go-to treatment. It’s been used since the 1950s and still works because it attacks the fungus directly without affecting your body’s other systems. It comes as a liquid suspension you swish in your mouth. Here’s how to use it right: Take 4 to 6 milliliters (about a teaspoon) four times a day-after meals and before bed. Swish it around for at least two minutes. Don’t swallow it right away. Let it coat your tongue, cheeks, and throat. Then spit it out. Swallowing it defeats the purpose-nystatin isn’t meant to be absorbed. It works locally. Studies show it cures mild to moderate thrush in 92% of cases when used correctly. But here’s the catch: 42% of people fail treatment because they don’t swish long enough. One Reddit user, "AsthmaWarrior42," said the chalky taste made it hard to stick with the four-times-a-day routine. But if you skip doses or rush through the swishing, the fungus comes back. It’s safe for kids, seniors, and pregnant women because almost none of it enters your bloodstream. Generic nystatin costs around $16 for a 30-day supply-much cheaper than alternatives.
Fluconazole: When You Need Something Stronger
If nystatin doesn’t work, or if your thrush is severe or spreading into your throat, your doctor will likely switch you to fluconazole (brand name Diflucan). This is an oral pill that your body absorbs. It works systemically, meaning it hits the fungus wherever it is. The usual dose is 100 to 200 mg once a day for 7 to 14 days. It’s fast-peak levels hit your blood in under two hours. Success rates are high: 95% of patients clear the infection. That’s why it’s the standard for people with weakened immune systems, like transplant recipients or those on chemotherapy. But it’s not without risks. Fluconazole can interact with 32 common medications, including blood thinners like warfarin, seizure drugs like phenytoin, and diabetes pills. It can also cause headaches, stomach upset, and, rarely, liver damage. One PatientsLikeMe user reported hospitalization after developing fluconazole-induced liver toxicity. That’s why your doctor will check your liver function before prescribing it. Cost-wise, generic fluconazole runs about $23 for a two-week course. Brand-name Diflucan? Over $300. There’s no reason to pay that unless you have no other option.Which One Should You Choose?
It’s not about which drug is "better." It’s about which fits your situation.- Choose nystatin if: You’re otherwise healthy, have mild thrush, are pregnant, take other medications, or are a child or senior. It’s safer, cheaper, and just as effective for simple cases.
- Choose fluconazole if: Your thrush is severe, didn’t respond to nystatin, has spread to your esophagus, or you’re immunocompromised. It’s faster and stronger-but only when you need it.
Prevention: The Real Key
Treatment helps-but prevention stops it from coming back. If you’re on an inhaled steroid, rinse your mouth with water immediately after each use. That simple step cuts your risk by 65%, according to NHS data. Brush your teeth twice a day. Floss daily. Clean your dentures every night if you wear them. Avoid sugary foods and drinks-Candida feeds on sugar. If you have diabetes, keep your HbA1c under 7.0%. High blood sugar is a direct invitation for thrush. New research shows promise in prevention beyond the basics. Probiotics like Lactobacillus reuteri can reduce recurrence by 57% when taken alongside antifungal treatment. Xylitol gum or lozenges also help-they reduce Candida colonization by 40%. And here’s something new: In March 2023, the FDA approved a new nystatin tablet called Mycolog-II that sticks to your mouth for up to four hours. It’s a game-changer for people who can’t stick to the swishing routine. It’s not widely available yet, but it’s a sign of where treatment is headed.