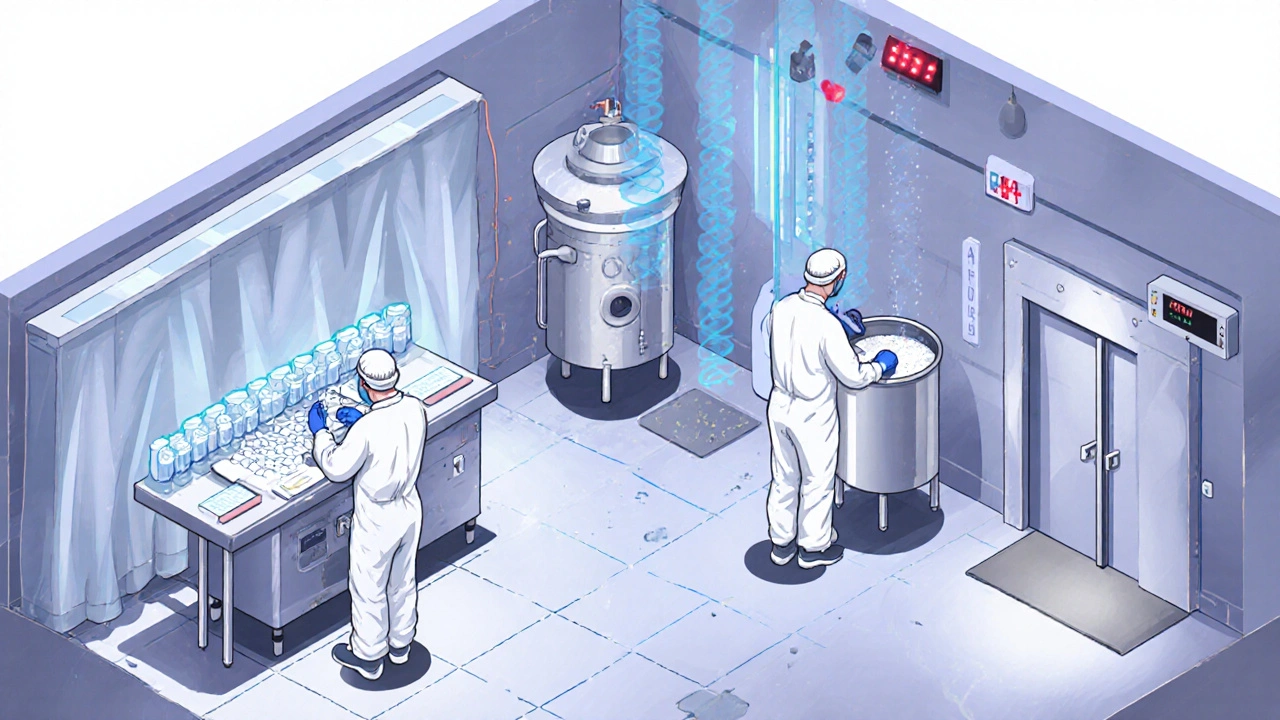
When you take a generic pill, you expect it to work just like the brand-name version. But behind that simple promise is a complex, tightly controlled environment you never see: the cleanroom. For generic drug manufacturers, meeting cleanroom standards isn’t optional-it’s the difference between a safe, effective medicine and a dangerous failure. These aren’t just clean spaces. They’re engineered systems designed to keep out particles, microbes, and human error that could ruin an entire batch of medication.
Why Cleanrooms Matter for Generic Drugs
Generic drugs are supposed to be identical in quality, strength, and performance to their brand-name counterparts. But here’s the catch: the brand-name drug was made in a facility built with unlimited budgets and decades of R&D. The generic version? Often made in a factory operating on 15-20% profit margins. That’s why cleanroom standards exist-to level the playing field. Without strict controls, even tiny contaminants can change how a drug behaves in your body. The FDA and European regulators don’t just want the chemical formula to match. They need the entire manufacturing process to be equivalent. That means the air you breathe in a cleanroom, the way workers dress, the airflow patterns, and even the humidity levels all become part of the drug’s quality. A single particle in the wrong place can lead to a recall. In 2022, the FDA issued 228 warning letters for cGMP violations-63% of all warning letters that year. Nearly half of those were tied to environmental monitoring failures in sterile generic drug production.The Four Cleanroom Grades Explained
Cleanrooms aren’t one-size-fits-all. They’re divided into four grades, each with exacting rules for particles, airflow, and microbial limits. These aren’t arbitrary numbers. They’re based on decades of science and real-world contamination events.- Grade A (ISO Class 5): The most critical zone. Used for filling sterile products like injectables. No more than 3,520 particles ≥0.5μm per cubic meter. Air moves in a smooth, unidirectional flow at 0.36-0.54 m/s. Think of it like a laminar airflow curtain that pushes contaminants away from the product. Temperature is kept at 18-26°C, humidity at 30-60%.
- Grade B (ISO Class 5 at rest, ISO Class 7 operational): The background area for Grade A. It’s where you prepare materials before they enter the critical zone. At rest, particle limits match Grade A. During operations, it can rise to 3.5 million particles. Continuous monitoring is required.
- Grade C (ISO Class 7 at rest, ISO Class 8 operational): Used for less critical steps like mixing powders or packaging. Particle limits jump to 3.5 million at rest and 35 million during operations. Still requires 20+ air changes per hour.
- Grade D (ISO Class 8 at rest): The least controlled zone. Only used for initial processing or storage. No operational particle limits, just 10 air changes per hour. Often the entry point for personnel before gowning.
How Cleanrooms Work: Air, Filters, and Pressure
Cleanrooms don’t stay clean by accident. They’re built with physics in mind. The key is airflow control. All cleanrooms use HEPA filters-H13 or H14 class-that capture 99.95% to 99.995% of particles as small as 0.3 micrometers. That’s smaller than most bacteria. But filters alone aren’t enough. Airflow direction matters. In Grade A zones, air flows straight down in a laminar pattern, like a silent waterfall. This pushes particles away from the product and out through floor grates. Pressure differentials are equally critical. Grade A rooms are kept at 10-15 Pascals higher pressure than Grade B. Grade B is higher than Grade C, and so on. This ensures that if a door opens, air flows out-not in. Contaminants from a dirty hallway can’t sneak in. Temperature and humidity are tightly controlled too. Too dry, and static electricity builds up, pulling particles onto surfaces. Too humid, and mold grows. The sweet spot? 18-26°C and 30-60% humidity. In tropical countries, adding dehumidifiers can increase HVAC costs by 20-30%.
Human Error: The Biggest Contamination Risk
You might think the biggest threat is a faulty filter. It’s not. It’s the person in the gown. Studies show that 42% of cleanroom deviations come from personnel gowning errors. A single sneeze can release 100,000 particles. A poorly sealed glove? That’s a direct path for skin flakes and bacteria into a vial of medicine. That’s why training isn’t optional. Workers spend 40-60 hours learning how to gown properly-step by step, with no shortcuts. They enter through airlocks, walk through sticky mats, and wear full-body suits with hoods, masks, and double gloves. Even then, movement is minimized. No quick turns. No unnecessary talking. Every motion is planned. One Pfizer facility manager described upgrading a generic oncology drug line from Grade C to Grade B. The HVAC upgrade cost $2.3 million and took 14 months. But it prevented 17 out-of-spec batches per year-each worth $500,000. The math was clear: the cost of failure was far higher than the cost of compliance.The Cost of Compliance: Who Pays the Price?
Building a Grade A cleanroom costs $250-$500 per square foot. For a 5,000-square-foot facility, that’s over $1 million just in construction. Add validation, training, monitoring systems, and ongoing maintenance, and the total can hit $3-5 million. For big pharma, that’s manageable. For a small generic manufacturer? It’s brutal. Many operate on 15-20% gross margins. Innovators? They make 70-80%. That’s why some small companies struggle. One Reddit user shared how maintaining Grade A for a $0.50-per-unit heparin syringe made the business unprofitable after a single FDA inspection flagged minor particle spikes. The global cleanroom market hit $3.7 billion in 2022, with generic manufacturers making up 38% of demand. But compliance costs represent 15-25% of a generic facility’s capital spend-compared to 10-15% for innovators. In India, upgrading to EU Annex 1 standards costs an average of $4.2 million per facility. In the U.S., it’s $2.8 million. Why? Infrastructure gaps. Older buildings, unstable power, water quality issues-all make compliance harder and more expensive.
Real Consequences: When Cleanrooms Fail
The 2012 New England Compounding Center outbreak killed 64 people and sickened over 750. The cause? Mold and bacteria in a poorly controlled cleanroom. That single failure changed the entire industry. More recently, in 2022, Aurobindo Pharma faced a $137 million recall of sterile injectables after FDA inspectors found inadequate Grade B monitoring. Their cleanroom had particle counts above limits, but no one was watching closely enough. The FDA issued a consent decree-meaning the company had to pay for independent audits for years. On the flip side, Teva’s generic version of Copaxone was initially rejected because of contamination events. After installing isolator technology in Grade A areas, contamination dropped from 12 events per year to just 2. The FDA approved it. That’s the power of getting it right.What’s Changing Now?
Cleanroom standards aren’t static. The EU’s 2023 revision of Annex 1 demands continuous air monitoring-not just periodic sampling. It also requires a full contamination control strategy, not just checklists. The FDA is moving in the same direction. New technologies are helping. AI-powered monitoring systems can detect airflow disruptions in real time. Robotics are replacing humans in high-risk zones. Single-use systems reduce cleaning needs. McKinsey predicts automation will cut cleanroom operational costs by 25-30% by 2028. But new challenges are rising. Biosimilars and complex generics like inhalers need more than standard cleanrooms. The FDA now projects that 50% of new generic applications by 2025 will require Grade A/B environments-up from 35% in 2022.What You Should Know
You don’t need to understand HEPA filters or particle counts to take your medication. But you should know this: every generic drug you take passed through a highly controlled environment designed to protect you. That’s not luck. It’s regulation, science, and hard work. If you’re a patient, trust that these standards exist for a reason. If you’re in the industry, know that cutting corners doesn’t save money-it risks lives. And if you’re wondering why generic drugs cost less than brand names? It’s not because they’re made in garages. It’s because manufacturers are squeezed to make them affordable-while still meeting the same gold-standard cleanroom rules.What is the main purpose of cleanroom standards in generic drug manufacturing?
The main purpose is to prevent contamination from particles, microbes, and human error that could compromise the safety, potency, or effectiveness of generic drugs. Since generics must be bioequivalent to brand-name drugs, even minor environmental flaws can lead to product failure, recalls, or harm to patients. Cleanroom standards ensure consistent, high-quality production regardless of the manufacturer.
How do Grade A and Grade B cleanrooms differ?
Grade A is the highest classification, used for direct product contact like filling sterile vials. It requires no more than 3,520 particles ≥0.5μm per cubic meter, unidirectional airflow, and constant monitoring. Grade B serves as the background environment for Grade A operations. At rest, it meets Grade A standards, but during operations, it allows up to 3.5 million particles. Grade B still requires continuous monitoring and strict gowning procedures, but it’s not the direct production zone.
Why are cleanroom standards stricter for sterile products like injectables?
Sterile products enter the bloodstream directly, bypassing the body’s natural defenses. Even a single microbe can cause a life-threatening infection. Oral pills pass through the digestive system, which can neutralize many contaminants. But an injectable? There’s no second chance. That’s why Grade A and B environments are mandatory for sterile generics, with real-time particle and microbial monitoring.
Do all generic drugs need the same level of cleanroom control?
No. Sterile products like injections, eye drops, and IV solutions require Grade A/B environments. Non-sterile products like tablets and capsules can be made in Grade C or even Grade D areas. However, even for oral solids, regulators are increasing scrutiny. Some experts argue Grade C is overkill for simple tablets, but recent FDA trends show tighter controls are coming across the board.
What happens if a generic drug manufacturer fails a cleanroom inspection?
Failure can lead to a Form 483 (inspectional observation), a warning letter, import alerts, or a consent decree. In severe cases, products are recalled-sometimes millions of units. Aurobindo’s 2022 recall cost $137 million. The FDA can also block future shipments until the facility fixes all issues. For small manufacturers, this can mean bankruptcy. The cost of compliance is high, but the cost of failure is catastrophic.
Are cleanroom standards the same worldwide?
They’re largely harmonized but not identical. The EU’s Annex 1 explicitly defines ISO classes for each grade. The FDA doesn’t use ISO labels in regulations but enforces equivalent controls. Japan requires additional monitoring at 1.0μm particle size. India and other emerging markets often struggle to meet EU standards due to infrastructure limits. Still, most major markets accept each other’s inspections under ICH guidelines, making global compliance a priority.